 Informal or unpaid caregivers (family members or friends) are the backbone of long-term care provided in people’s homes. While some aspects of caregiving may be rewarding, caregivers can also be at increased risk for negative health consequences. These may include stress, depression, difficulty maintaining a healthy lifestyle, and staying up to date on recommended clinical preventive services.
Informal or unpaid caregivers (family members or friends) are the backbone of long-term care provided in people’s homes. While some aspects of caregiving may be rewarding, caregivers can also be at increased risk for negative health consequences. These may include stress, depression, difficulty maintaining a healthy lifestyle, and staying up to date on recommended clinical preventive services.
Caregiving is hard work. Failing to plan for the future ensures that it will be even more difficult for whoever helps you if you need a caregiver.
Informal or unpaid caregiving has been associated with:
- Elevated levels of depression and anxiety
- Higher use of psychoactive medications
- Worse self-reported physical health
- Compromised immune function
- Increased risk of early death
Rosalynn Carter said it first and she said it best: “There are only four kinds of people in the world: those who have been caregivers, those who are currently caregivers, those who will be caregivers, and those who will need caregivers.”
Caregivers can be spouses, partners, adult children, parents, other relatives (siblings, aunts, nieces/nephews, in-laws, grandchildren), friends, neighbors. They don’t start off planning to be caregivers. It just happens. Caregivers often have employment and family obligations in addition to caregiving. They usually burn the candle at both ends.
Caregivers need a plan. But how do you develop a care plan? Start a conversation about care planning with the person you take care of. You can use the “My Care Plan” form to help start the conversation. If your care recipient isn’t able to provide input, anyone who has significant interaction with the care recipient (a family member or home nurse aide) can help complete the form. Talk to the doctor of the person you care for or another health care provider. A physician can review your plan and help to refine it, especially if there is a conversation about advanced care planning. Ask about care options that are relevant to the person you care for.
Medicare covers appointments that are scheduled to manage chronic conditions and for discussing advanced care plans. Beginning in January of 2017, Medicare covers care planning appointments specifically for people with Alzheimer’s, other dementias, memory problems, or suspected cognitive impairment. Discuss any needs you have as a caregiver. 84% of caregivers report they could use more information and help on caregiving topics especially related to safety at home, dealing with stress, and managing their care recipient’s challenging behaviors. Caregivers of people with dementia or Alzheimer’s are particularly at greater risk for anxiety, depression, and lower quality of life compared to caregivers of people with other chronic conditions.
Caregivers need help. They are living in the midst of a storm. When you meet one, your first question should always be “how can I help.” We will continue to add resources as this site grows, but in the meantime, there are many podcast episodes you can listen to on our Caregiving Podcast page. As membership grows here, you can use our Caregiver Forum to ask other caregivers how they dealt with specific problems.
Caregivers must accept help. Do not allow yourself to get burned out. If you burn out, who will replace you? If you get burned out, will your loved one be able to live independently? Build a team and realize that anything that can be done by someone else can be delegated. Your team should include planners, schedulers, doer’s, encouragers and financiers. For example, if one sibling is out of town and cannot help with hands on caregiving, then he or she can still encourage or help manage a parent’s finances. Someone can use a family organizer app to help keep track of appointments and important events. See FCA’s Tips for Taking Care of You.
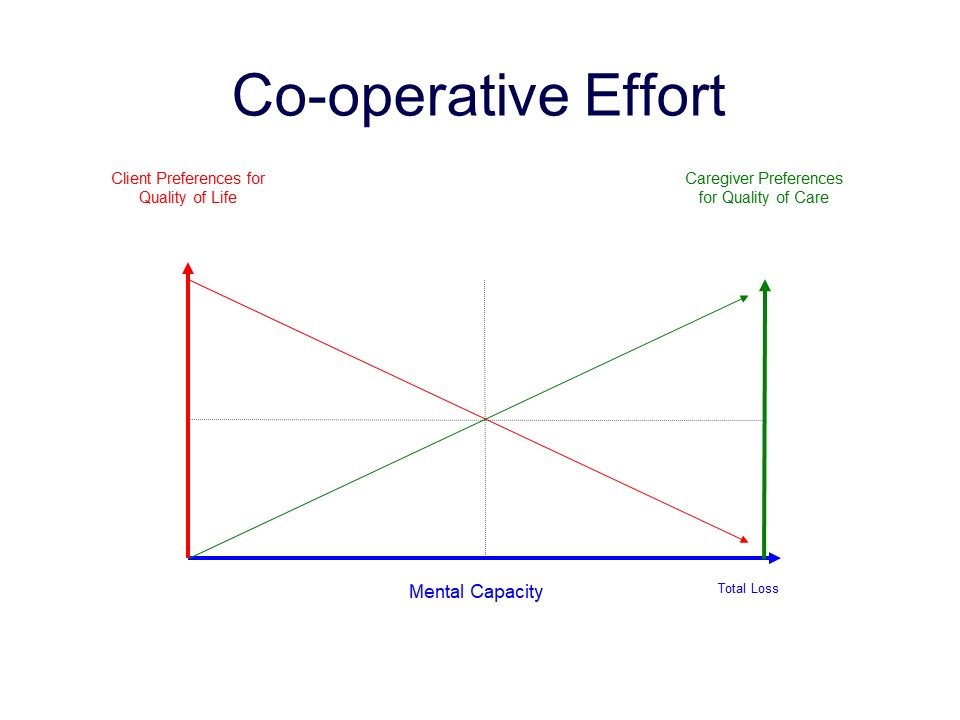
Caregivers must have boundaries. If you refuse to set boundaries, you will burn out. Your other relationships will suffer. You will lose yourself. Boundaries are healthy because in setting them, you must admit your inability to be everything and do everything. Further, although the preferences and dignity of the person being cared for should be respected, you must remember that caregiving is a “team sport.” As the cognitive abilities of the person being cared for diminish, the caregiver’s preference regarding how care is provided will become more significant. So long as the person needed care is treated with dignity and respect, there is nothing wrong with looking after yourself. As one writer said:
When you’re driving down the road, street signs and road markers can help you know if you’re on the right track, while creating boundaries that allow traffic to move efficiently and safely. When you’re dealing with people, however, it can be a little bit harder to set up those boundaries, … A key part of learning when to say “no” ultimately comes down to setting and recognizing your limits. This includes the “internal” limits that you must set for yourself, and the “external” boundaries that you’d like to keep up with the people in your life, including your senior loved one and the other members of your family, as well as healthcare providers and professional caregivers.
When dementia is involved, the caregiver burden is elevated. Dementia not only robs the individual of his or her ability to help, it robs them of the ability to be grateful. In other words, the work increases while the “thank you’s” disappear.
How do you begin as a caregiver? First, make an honest assessment of your loved one’s needs and your ability (or inability) to meet those needs. Ask other family members for help.
Exacerbating the caregiver problem is distance. American families frequently spread out. If some children remain geographically close to aging parents, chances are they are alone and the caregiver burden falls disproportionately on him or her. If you find yourself in this situation, you should download the Family Caregiver Alliance’s Handbook for Long-Distance Caregivers. Firms that assist families with payroll and worker’s compensation solutions for in-home paid caregivers are linked on EZ Elder Law’s resources page under the heading “Caregiving.”
Eldercare Locator, 1-800-677-1116 (toll-free)
Family Care Navigator, 1-800-445-8106 (toll-free)
Additional Resources:
- Rosalynn Carter Institute for Caregivers
- Caregiving.com
- 2020 Caregiving in the U.S. Report from AARP and NAC
- AARP Caregiver Resources
- Caregiver 101 (Family Caregiver Alliance)
- Advocacy Tips for Family Caregivers (Family Caregiver Alliance)
- Caregiver College Video Series (Family Caregiver Alliance)
- IRS Publication 926 – Household Employer’s Tax Guide
- Georgia Family Caregiver Support Act, O.C.G.A. § 49-6-70 et seq.
BLOG POSTS
Generational Cohorts
Researchers use generational cohorts to identify and analyze changing views over time. A typical generation spans 15 to 18 years and when cohorts are compared, there is often great diversity of thought, experience and behavior. In The Whys and Hows of Generations Research, the Pew Research Center said an “individual’s age is one of the […]
Moratorium on Nursing Home Staffing Standards
Moratorium on Nursing Home Staffing Standards On July 4, 2025, the One Big Beautiful Bill Act was signed into law. One of its provisions placed a moratorium on the Biden Era minimum staffing standards for nursing homes. Specifically, Section 71111 of the OBBBA provides: Subchapter B—Preventing Wasteful Spending SEC. 71111. MORATORIUM ON IMPLEMENTATION OF RULE […]
ADLs and IADLs
ADLs and IADLs Activities of Daily Living and Instrumental Activities of Daily Living describe basic skills for getting through the day. Sidney Katz is credited as the first to use this term in 1950. “The ability to perform activities of daily living (ADL), such as bathing or dressing, instrumental activities of daily living (IADL), like […]
Planning for Adult Children with Disabilities
Planning for Adult Children with Disabilities Childhood Disability Benefits assist disabled children and adults who became disabled prior to age 22. Most begin with Supplemental Security Income, which is a monthly cash payment for individuals with limited income and few resources. Because a parent’s income and resources are usually deemed available to the child, SSI […]
The ARC Fights to Protect Medicaid
Medicaid is critical for individuals with special needs. It pays for things no one else will pay for and it has recently come under fire. The Arc is working to protect Medicaid for its constituents. It is activating advocates to protect services for the disability community. It is also seeking donations to further its efforts. […]
Pat Summitt Documentary
If you follow Women’s College Basketball, then you must have heard of Pat Summitt. Coach Summit was a legend in NCAA women’s basketball prior to leaving the game due to early-onset Alzheimer’s disease. Now, there is a rumored new documentary on Netflix that recounts her journey from player to becoming a legend at the University […]
Service Animals and the ADA
Service animals used by individuals with a disability can only be excluded from public places if they cannot be controlled by their handler or if they are not house broken. See Title II, Section 35.136. Usually service animals must be harnessed, leashed or tethered unless the individual’s disability prevents using those devices or unless it […]
Americans with Disabilities Act of 1990: The Basics
On July 26, 1990, President George H.W. Bush signed into law the Americans with Disabilities Act of 1990 (“ADA”), a comprehensive civil rights law prohibiting discrimination on the basis of disability. The law was amended on September 25, 2008, when President George W.Bush signed into law the Americans with Disabilities Amendments Act of 2008 (ADA […]
Award of Custody to Grandparent Overturned
Award of Custody to Grandparent Overturned In Geiger v. Allmond, 371 Ga. App. 641 (May 23, 2024), the Court of Appeals reversed a trial court decision awarding custody of two minor children to their paternal grandmother. Several cases were consolidated on appeal. Ashely Geiger, the mother, appealed the award of custody to Patti Allmond, the […]
Guiding an Improved Dementia Experience (GUIDE) Model for Dementia Care
The Centers for Medicare and Medicaid Services launched the Guiding an Improved Dementia Experience (GUIDE) Model on July 1, 2024. It is a voluntary nationwide model test that aims to support people with dementia and their unpaid caregivers. The GUIDE Model is an attempt to provide Medicare funded comprehensive, coordinated dementia care to improve quality […]
Medicaid’s Refusal to Provide 24/7 Care in the Community Might be Discrimination
Medicaid’s Refusal to Provide 24/7 Care in the Community Might be Discrimination In Harrison v. Young (5th Cir. June 6, 2024), the Fifth Circuit considered Ms. Barbara Harrison’s claim challenging Medicaid‘s denial of funding for medical services that she claimed are necessary for her survival. Harrison has severe physical and intellectual disabilities. She cannot walk […]
Updates to Nursing Home Quality of Care Regulations
From time to time federal regulations covering nursing home quality of care are updated. Thus far, the following updates have been published in May and June of 2024. Updates posted May 10, 2024 42 CFR Part 483 — Requirements for States and Long Term Care Facilities view changes § 483.5 Definitions. view changes § 483.10 […]
Federal Nursing Home Quality of Care Regulations
Nursing homes that accept Medicare or Medicaid are required to comply with quality of care regulations. Although we have blogged elsewhere on specific nursing home resident rights, the current federal regulations are linked below. 42 CFR Part 483 — Requirements for States and Long Term Care Facilities § 483.5 Definitions. § 483.10 Resident rights. § […]
Virtual Dementia Tour
Dementia affects more than 50 million people worldwide. The Virtual Dementia Tour is designed to allow participants to experience what dementia patients see, hear and feel so they better understand and empathize with individuals who have dementia. One website with the UNC Greensboro reports: “The simulation temporarily alters your physical and sensory abilities to replicate […]
New Report cites dangers in relying on data regarding quality of care in Assisted Living Facilities
In February 2024, Justice in Aging released a new report based on California’s “performance measure” data from the state’s Medicaid assisted living program. Aging in Justice concluded that the quality of care measures provide no meaningful information. A perfect score tells you nothing about the quality of care residents receive. The report concludes that the […]
Georgia Adult Protective Services Manual
Georgia Adult Protective Services Authority for Adult Protective Services is found at O.C.G.A. § 30-5-1 et seq. The stated purpose of the Act ” is to provide protective services for abused, neglected, or exploited disabled adults and elder persons. It is not the purpose of this chapter to place restrictions upon the personal liberty of […]
Sometimes You Must Say No
Sometimes you just have to say No “No” isn’t a four-letter word. Saying “no” isn’t necessarily bad and you shouldn’t feel bad when you say it. Part of saying no means taking a stand. It can mean standing up to injustice. For example, our legal system is, for the most part, dependent on people saying […]
Why People Do What They Do?: A Desire for Certainty
This is the first in a series of posts exploring why people do what they do. In this post, we’re discussing certainty. When I was a young lawyer, I worked on a corporate team where Fortune 500 companies paid tens of thousands of dollars for certainty. When they signed a contract, they wanted to know […]
Do Hearing Aids Slow Mental Decline and Dementia? A New Study Says They Do
Aging and Cognitive Health Evaluation in Elders (ACHIEVE) is a landmark study of the effect of hearing intervention on brain health in older adults. Findings, recently published in Lancet, showed that hearing loss is associated with cognitive decline and one goal was to determine whether hearing intervention could reduce cognitive decline. ACHIEVE’s key findings showed […]
Wednesday Morning Walk – July 19, 2023
Brother Allen Byers spoke from Genesis 21, beginning at verse 11. The message, called Slow Down To Look Around, tells us that it’s not our responsibility to make God’s promises come true. Yes, we’re supposed to obey God and avoid laziness, but God will make His own promises come true. Listen HERE.
Upcoming Senior Events in Northwest Georgia
As of the date of this post, the following events are upcoming in Northwest Georgia: Saturday, July 22nd – Phil Wilson’s “7th Annual Float For Hope”. An Alzheimer’s Association benefit. Starting at 11am at Grizzard Park. $10 per person. Raffle tickets are available and an after party at River Remedy! Saturday, July 22nd – The Fountains in […]

Leqembi Approved by FDA
The FDA has approved Leqembi (Lecanemab) for patients with mild dementia and other symptoms caused by early Alzheimer’s disease. Approval followed a determination that a confirmatory trial verified clinical benefit. Leqembi is the first amyloid beta-directed antibody to be converted from an accelerated approval to a traditional approval for the treatment of Alzheimer’s disease. In […]

Relationships and Information Overload
Here are a few stats: The average shopper sees 4,000 ads in a day. The average person is interrupted once every 8 minutes. On average, people spend 3 hours and 15 minutes per day on their phones. The typical American spends three hours per day watching TV. The stats on prayer aren’t quite as good. […]
Getting Health Care Directives to Your Doctors FAST
If you are in the midst of a crisis, it’s critical for doctors and other health care providers to know who to listen to and who can make decisions. Obviously, if it’s your regular physician, the ideal solution is to give him or her a copy of your health care advance directive and have it […]

Federal Holidays
The Office of Personnel Management maintains a page listing all federal holidays. If the holiday falls on a Saturday, then the holiday is observed on the preceding Friday. If the holiday falls on a Sunday, then it is observed on the following Monday. In 2023, the following federal holidays will be observed: Date Holiday Monday, […]

Elder Law Mishmash June 2023
The following is a mishmash of information on various Elder Law, Special Needs Law, and Estate Planning issues. It also includes anything else we found interesting during the month of June, 2023. We will continue updating from time to time throughout the month. Last updated 6/8/2023. Keep in mind, you are using linked content at […]

Employees versus Independent Contractors
Many families get this issue confused, but it’s serious business for the IRS. In Cardiovascular Center, LLC v. Commissioner of Internal Revenue (U.S. Tax Court 5-18-2023), Dr. Frank Kresock operated a medical practice in Arizona. He paid four workers, plus the person he lived with, as independent contractor’s, giving them biweekly cashier’s checks. However, all […]

Wednesday Morning Walk, May 17, 2023
On Wednesday, May 17, 2023, Allen Byers spoke from Matthew, Chapter 8, about Jesus and the Centurion. This story comes from verses 5 through 13, There, the Bible says And when Jesus was entered into Capernaum, there came unto him a centurion, beseeching him, And saying, Lord, my servant lieth at home sick of the […]

You Are Enough
Caregiving is hard. Being a parent is hard. Being a child is hard. And sometimes you might feel like you’re not enough. You are enough and you need to listen to this song. You’re enough!

VA Announces Legal and Financial Planning Services are Now Available for Family Caregivers
On April 25, 2023, the VA issued the following announcement: The Caregiver Support Program (CSP) is introducing a new nationwide service offering comprehensive legal and financial planning services to Primary Family Caregivers enrolled in the Program of Comprehensive Assistance for Family Caregivers (PCAFC). A network of licensed attorneys and certified financial counselors are readily accessible […]

Biden Whitehouse Issues Executive Order to Increase Access to Care and to Support Caregivers
On April 18, 2023, the Biden Whitehouse issued an Executive Order on Increasing Access to High-Quality Care and Supporting Caregivers. The EO directs actions to improve job quality for the professionals who provide the critical services that make community living possible for millions of people. It includes actions to improve support for the 53 million […]

VA posts regarding its Comprehensive Assistance for Family Caregivers
On April 5, 2023, the VA posted (presumably to remind everyone) regarding its comprensive assistance for family caregivers. The VA said “Support for caregivers means making sure you’re informed about the programs, resources, and services available to you. The Caregiver Support Program (CSP) provides clinical services to caregivers of Veterans who are enrolled in the […]

Ruminations on Care and Care Planning
At this point, there are many companies and services out there claiming to provide care and care planning. So what’s that all about, and what’s the difference between care and care planning? Essentially, care is a service where someone comes to your home, or another place where you need help, and provides care. Usually a […]

What is CareTree?
Many years ago, I helped found an organization called the Life Care Planning Law Firms Association. Since then many companies have tried to mimic what law firms do, often with disastrous consequences. Recently, we ran across a website that appears to be different and might actually be helpful. It’s called CareTree.me. This website says it […]

Advocates Academy: My Dream
My dream is to establish an advocate’s academy. The ultimate name isn’t as important as the mission. It will train existing and future leaders in law, medicine, faith, government, law enforcement, education, caregiving and more. The goal is to develop leadership skills, discuss ethics, improve professionalism, and expand the knowledge base for attendees in their […]

ABLE Accounts
The Achieving a Better Life Experience (ABLE) Act of 2013 (S. 313/H.R.647) was introduced in the 113th Congress by a bipartisan group of Congressional Champions that included Sens. Robert Casey, Jr. (D-PA) and Richard Burr (R-NC), and Reps. Ander Crenshaw (R-FL), Chris Van Hollen (D-MD), Cathy McMorris Rodgers (R-WA) and Pete Sessions (R-TX). The ABLE […]

New Hospice Resource
On December 9, 2022, the Center for Medicare Advocacy and the National Association for Home Care & Hospice announced development of a new hospice resource. The resource is entitled “Questions to Ask When Choosing a Hospice.” You can access this resource on the CMA page or the NAHCH page.

The Dignity Account
One of the issues families consider as loved ones age is whether an elder is susceptible to financial elder abuse. When trying to protect mom or dad (or another elderly loved one), sometimes famlies overstep. Paternalism is not appropriate when an elder is capable of making his or her own decisions; if the elder has […]

Elder Law and Special Needs Law News Roundup – 10-21-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]

Elder Law and Special Needs Law News Roundup – 10-14-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]

Elder Law and Special Needs Law News Roundup – 9-30-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]

Chronic Care Model and Patient Advocacy
In the late 1990s, Dr. Ed Wagner (and his team at the Macccoll Center – now the ACT Center), created the Chronic Care Model for the delivery of care. They had the support of the Robert Wood Johnson Foundation. The chronic care model recognizes that when care is delivered over time, patient involvement becomes increasingly […]

Elder Law and Special Needs Law News Roundup – 9-23-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]

HHS Delivers First National Strategy to Support Family Caregivers
On September 21, 2022, the U.S. Department of Health and Human Services (HHS), through its Administration for Community Living (ACL), released the 2022 National Strategy to Support Family Caregivers . It highlights nearly 350 actions the federal government will take to support family caregivers in the coming year and more than 150 actions that can […]

Update on Talevski v. Health and Hospital Corporation of Marion County
In our August 26, 2022, News Roundup, we reported that Talevski v. Health and Hospital Corporation of Marion County (HHC) was headed to the Supreme Court. The case concerns the rights of nursing home residents. The Plaintiff argued the nursing home violated his rights under the Federal Nursing Home Reform Act (FNHRA). The nursing home […]

Elder Law and Special Needs Law News Roundup – 9-16-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]

Elder Law and Special Needs Law News Roundup – 9-9-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]

Cognitive Rehab May Help Older Adults Clear Covid-Related Brain Fog
By: Judith Graham August 5, 2022 Eight months after falling ill with covid-19, the 73-year-old woman couldn’t remember what her husband had told her a few hours before. She would forget to remove laundry from the dryer at the end of the cycle. She would turn on the tap at a sink and walk away. […]

Articles – Week of September 9, 2022
We regularly scour the internet looking for information relating to elder care, special needs and elder law. Although we review a number of sources collecting information, many of the articles listed here were found using Google Scholar Alerts. If a link you need has gone missing, try pasting the link into the Wayback Machine (Internet […]

Elder Law and Special Needs Law News Roundup – 9-2-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]



