“Long-term care covers a diverse array of services provided over a sustained period of time to people of all ages with chronic conditions and functional limitations. Their needs for care range from minimal personal assistance with basic activities of everyday life (ADLs) to virtually total care.” Institute of Medicine, Improving the Quality of Long-Term Care, p.36 (National Academy Press 2001). Long-term care is typically how we help those with functional deficits cope between acute care situations (i.e. doctor visits). It is a day-in-day-out process.
Long-term care is designed to meet a person’s health or personal care needs during a short or long period of time. LTC services help people live as independently and safely as possible when they can no longer perform everyday activities on their own. Long-term care is provided in different places by different caregivers, depending on a person’s needs. Most long-term care is provided at home by unpaid family members and friends. It can also be given in a facility such as a nursing home or in the community, for example, in an adult day care center.
It is difficult to predict how much or what type of long-term care a person might need. Several things increase the risk of needing long-term care.
- Age. The risk generally increases as people get older.
- Gender. Women are at higher risk than men, primarily because they often live longer.
- Marital status. Single people are more likely than married people to need care from a paid provider.
- Lifestyle. Poor diet and exercise habits can increase a person’s risk.
- Health and family history. These factors also affect risk.
Unfortunately, health care often fails to meet the needs of chronically ill people. Treatment regimens for chronic illness often do not conform to evidence-based guidelines. Care may be rushed and overly dependent on patient-initiated follow-up. In part, recognition of these problems resulted in development of the Chronic Care Model at the Improving Chronic Illness Care program at the MacColl Center for Health Care Innovation. That model identified the “informed, activate patient” (or surrogate) as an essential element of the chronic care team.
Here are several thoughts concerning what good long-term care should look like. First, good care should be planned. Each patient should have a medical home. Each patient should adopt his or her own set of goals concerning quality of life and that this should be done in a context separate from the treating health care provider to eliminate any appearance of conflict. Good planning should begin early and should incorporate the patient’s values.
Second, long-term care should be accessible. If a patient cannot access care, then needs remain unmet. Unmet needs will result in danger zones where the need for additional care and loss of function can accelerate.
Third, long-term care should be proactive. Do not wait until an injury occurs to develop a plan for providing care. Whether a particular plan is put into effect may be a function of patient choice, but care should be forward-looking and designed to minimize the likelihood that someone who is aging in place declines unnecessarily.
Fourth, long-term care should be systematic. This is not to say that individuality is ignored; it simply recognizes that many tasks associated with long-term care are routine and a system should be in place to ensure that care is provided as needed.
Fifth, care should be individualized. While the medical literature indicates that as we age, we become more different. We remain a society of “doer’s” rather than “listeners.” We focus on task efficiency, forgetting that we are dealing with people. Good care is not simply the absence of bad outcomes; it is the enhancement of quality of life.
Sixth and closely related to the fifth, care should involve the patient and should answer questions. Good care is interactive, invoking the informed consent process. Good communication and comprehensibility are essential to the process of involving the patient.
Seventh, care should be comprehensive, at least in the sense that it is holistic and meets the patient’s needs and desires. It should account for a person’s physical, mental and psycho-social well-being.
Eighth, good care should be measurable. There should be standards for determining whether care is meeting the needs of the individual and appropriate care should be provided at each instance when it is needed.
Ninth, long-term care should be consistent. Although consistency is related to measurability and systematic delivery, we believe this concept differs enough for separate discussion.
Finally, providers must be accountable to their patients. Accountability comes in many forms such as market choice – if a provider is non-responsive then the patient simply goes elsewhere. Accountability may take different forms such as through litigation. But in this context, we believe accountability means personalized care designed to ensure that outcomes are consistent with planning goals.
Other important principles include: health care should be affordable, cost efficient, and should seek to meet the needs of underserved populations.
Good care invokes not just consideration of what is done, but how, where and for how long it is done. These considerations take into account patient preferences as well as the preferences and abilities of caregivers. Overburdening caregivers results in burnout, which will cause the plan to fail. These considerations necessarily require exploration of what older people want from long-term care. Most elders want to remain home. They want to maintain independence for as long as possible, although the meaning of independence will vary from person to person. Also, most elders want to manage change.
Continuum of Care
Long-term care is provided over time as individuals with chronic illnesses decline in health. Most long-term care is provided at home by family members. When informal care is no longer possible, Elders enter the formal long-term care system. Individuals receiving long-term care tend to tread deeper into the Elder Care Continuum, rarely regaining lost function. On the shallow end the continuum is home, and those with no functional deficits or few care needs tend to be there. In the deepest part of the continuum, the patient needs total care. This tends to be nursing home care. Between these extremes, a panoply of options exists, some of which are described below.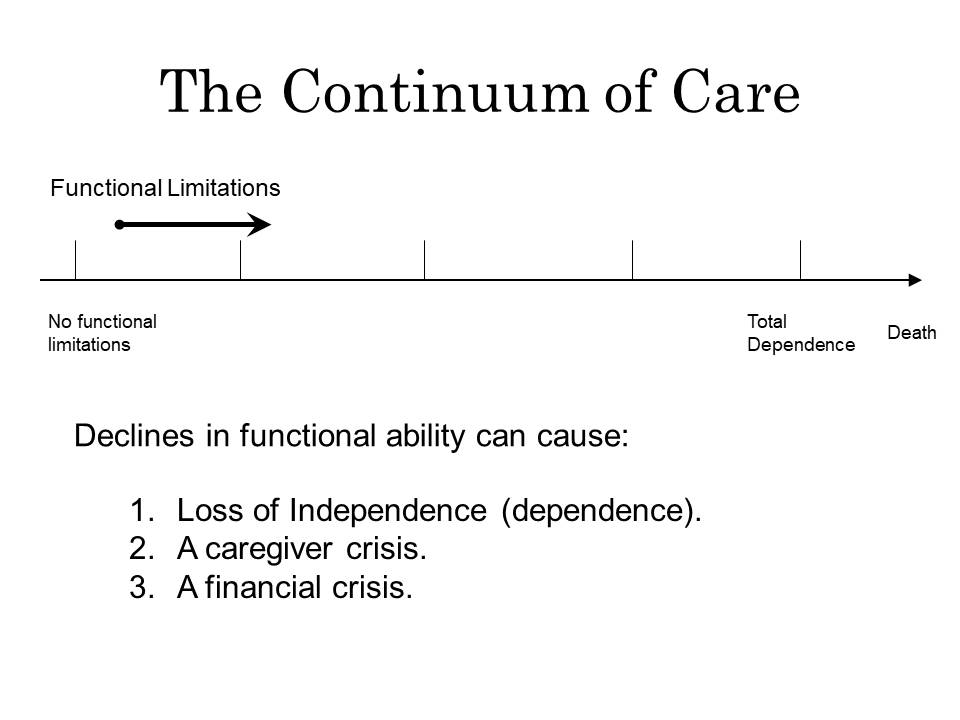
Home
Elders want to stay home. Home can mean anything, but generally speaking, it is where an individual chooses to live. Prior to functional loss, individuals tend to adapt to their environment. After onset of functional loss, the environment often times must adapt to the individual’s needs. When the physical environment can no longer be adjusted to meet the needs of the elder, then additional caregiver resources are required, or a change in environment may be necessary.
Most long-term care is provided at home by family and friends. Isolation, because the Elder is single or after loss of a spouse, can result in a move to a more formal setting. Other conditions leading to a change in housing situation include loss of the caregiver support system, need for assistance with medication management, fear of falling, falls resulting in injury, acute episodes coupled with fear of recurrence or with a decline in condition, wandering, and incontinence. The need for rehabilitation can result in a short-term stay away from home, with the average rehabilitation time being 30 to 40 days.
Home with Family Assistance
Most caregiving is done at home by family members. Most is unpaid. Family assistance can range from giving “mom” a ride to the doctor’s office to providing total care. Unless an elder is being abused, no law requires admission to a formal long-term care institution. However, statistics tell us that because caregiving is hard work, over time caregivers need assistance. Caregiver burnout is not uncommon. Caregivers tend to suffer deleterious mental health effects and from physical problems including increased blood pressure and insulin levels, impaired immune systems and in increase in cardiovascular disease. When the family network breaks down or, preferably before it breaks down, outside assistance should be summoned.
Personal Care Services
Many providers offer home-maker assistance and assistance with non-skilled needs. Services may include self-care assistance such as help with bathing, eating, dressing and toileting or household assistance which includes housekeeping, laundry, meal preparation, shopping and bill paying. Other services such as transportation, sitter/companion and medication monitoring are available. Services are generally available 24 hours a day seven days a week, although round-the-clock care would likely exceed the cost of nursing home care.
Home Health Care
Home health agencies provide skilled nursing and rehabilitative care such as physical, occupational and speech therapy. Often, agencies providing these services will provide ancillary personal services as well. These services are particularly important when the Elder requires regular medical care that is beyond the knowledge and experience of family caregivers.
Adult Day Care
These programs provide social activities, meals, assistance with personal needs, health education and supervision in a safe environment on a temporary basis. Most centers are open Monday through Friday during normal business hours and allow full-time caregivers an opportunity to continue their daily work and family routines while providing supervision and care for the elderly person.
Respite Care
Respite care offers relief for home caregivers by allowing overnight accommodations as well as medical and social supervision in a nursing home or an assisted living facility.
Homes for the Aged
These facilities are designed to provide a place where people who are able to care for themselves with little or no help, may receive room, board and limited personal services. Someone who lives in the home must be physically and mentally capable of finding his or her way out of the building in case of an emergency without the assistance of another person. They are neither staffed nor licensed to provide medical care. Depending on amenities, they may range from apartment style living to something that looks more like a country club.
Continuing Care Retirement Communities (CCRCs)
Continuing care retirement communities (CCRCs) offer seniors long-term contracts that guarantee lifelong shelter and access to specified health care services. In return, residents usually pay a lump-sum entrance fee and regular monthly payments. Depending on the contract, the entrance fee may be nonrefundable, refundable on a declining basis over time, partially refundable, or fully refundable. CCRC residents enjoy an independent lifestyle with the knowledge that if they become sick or frail, their needs will continue to be met, usually on-site. These communities provide a continuum of care from independent housing through skilled nursing care.
Assisted Living Residences
Assisted living is a long-term care option for Elders that is frequently built on a social, rather than medical, model. ALFs are for individuals who need some assistance, but do not require the nursing care provided in a nursing home. These facilities are regulated. Although regulations will differ from State to State, in many areas, they are allowed to help administer medications to the resident. Typically, there are no bed-bound residents.
Among those services provided at assisted living facilities are meal preparation, assistance with medication management, housekeeping, and standby assistance with bathing, dressing, and grooming. The routine provided in this setting will frequently contribute to improvement or stabilization of the resident’s condition. Frequently, home health care can provide therapy or other services in the assisted living home to extend a resident’s ability to stay. Residents who live in assisted living are usually required to transfer independently and must be able to exit the building independently during emergencies. Many assisted living facilities today operate under a hospitality model, leading some to compare them to a docked cruise ship. Residents who enter this level of care typically remain there for two to five years.
Typically, resident danger is associated with an improper admission or an untimely discharge. Proper care at this level will include a comprehensive assessment to determine whether an admission is appropriate (e.g., will the resident be safe) and will also establish a functional baseline. The facility should monitor the resident’s condition on a regular basis and if a decline in condition would put the resident in danger, then the resident should be discharged to a higher level of care. Conditions that typically result in the need for a higher level of care are the progression of dementia, or the need for skilled therapy. Counseling is frequently necessary when a resident must be discharged because either the resident or the resident’s family is in denial.
Memory Care Units
More and more assisted living facilities are establishing memory care units. These units operate on the same social model as other ALFs, but have locked units to prevent wandering.
Nursing Homes
The job of a nursing home is to provide 24-hour nursing care to those who are chronically ill or injured, have health care needs as well as personal needs and are unable to function independently. The team of caregivers in a nursing home includes the administrator, a physician who serves as the facility’s medical director, registered nurses, licensed practical nurses, certified nursing assistants, a dietitian, activity coordinator, social worker and housekeeping staff. Nursing homes may provide two levels of care: intermediate care and skilled care. Intermediate care is typically custodial, although it functions at a higher level than any other care setting. Skilled care provides the residents with more extensive services such as physical, occupational, speech or respiratory therapy. Many nursing homes have an Alzheimer’s unit which is typically secured.
One of the primary problems with nursing home care is the stigma attached to them. Many elders still envision them as the county “old folks home” or the “poor house.” Many people have an expectation that those admitted to a nursing home will get worse, or that a nursing home is a place to die. Sometimes these stigmas lead to depression, which in turn impacts recovery. One nursing home administrator indicated that the best way to confront these out-dated notions is by having people visit the nursing home. Many nursing homes have moved toward hotel style amenities and one administrator indicated that within ten years, consumers will expect nursing homes to deliver medical care “hotel-style.”
One nursing home administrator indicated that learning the resident’s story can contribute to better care. It personalizes the resident. For those who come into the nursing home cognizant, the staff can talk to the resident. For residents with dementia or other conditions that prevent dialog, it is important for family members to let the staff know who Mom or Dad were before their condition declined. “Local” nursing homes sometimes have an immediate bond with residents because staff members knew the resident prior to admission.
More data exists concerning the quality of nursing home care than any other level of care. This is because most nursing homes accept Medicare and Medicaid funds and, therefore, are subject to inspection and reporting requirements. According to the IOM Report “[e]vidence indicates that the quality of nursing home care in general has improved over the past decade, even though nursing homes are serving a more seriously ill population.” This appears to be consistent with other data, such as a GAO report from July 2003 titled Nursing Home Quality: Prevalence of Serious Problems, While Declining, Reinforces Importance of Enhanced Oversight. There, the GAO reported that the magnitude of problems uncovered during standard nursing home surveys remains a cause for concern even though OSCAR deficiency data indicates that state surveyors are finding fewer serious quality problems. Most of the serious survey deficiencies seem to be coming from the same underperforming nursing homes.
Hospice Care
Traditionally hospice care is provided at home. It is palliative care, not curative care, for the terminally ill. It addresses not only physical needs and pain management but also psychological, spiritual and emotional needs for residents, family members and friends. Hospice care is provided through an interdisciplinary, medically directed team. This team approach to care for dying persons typically includes a physician, a nurse, a home health aide, a social worker, a chaplain and a volunteer. Hospice requires a doctor’s order with a prognosis of 6 months. For those who qualify, hospice services are paid for by Medicare and the room and board at the nursing home is paid for privately or by Medicaid. The resident liability which is paid monthly to the nursing home is discontinued. Many times the family benefits more from the services than the resident.
Resources
Long Term Care (Administration on Community Living)
BLOG POSTS
There are only six legal reasons to discharge a nursing home resident
Valid Reasons for an Involuntary Nursing Home Discharge One thing that strikes fear in the hearts of families caring for loved ones in a nursing home is a notice of involuntary discharge. If the nursing home accepts Medicaid or Medicaid, or both, then there are only six legal reasons for an involuntary discharge. Since virtually […]
Moratorium on Nursing Home Staffing Standards
Moratorium on Nursing Home Staffing Standards On July 4, 2025, the One Big Beautiful Bill Act was signed into law. One of its provisions placed a moratorium on the Biden Era minimum staffing standards for nursing homes. Specifically, Section 71111 of the OBBBA provides: Subchapter B—Preventing Wasteful Spending SEC. 71111. MORATORIUM ON IMPLEMENTATION OF RULE […]
Long Term Care Services for Veterans
The Veteran’s Administration (the VA) makes long-term care support available for qualifying veterans in several ways. VA Community Living Centers (CLCs) CLCs are VA owned and operated. Veterans can receive nursing level care, including assistance with activities of daily living. Veterans are encouraged to make their rooms feel home-like by decorating their rooms and they […]
Updates to Nursing Home Quality of Care Regulations
From time to time federal regulations covering nursing home quality of care are updated. Thus far, the following updates have been published in May and June of 2024. Updates posted May 10, 2024 42 CFR Part 483 — Requirements for States and Long Term Care Facilities view changes § 483.5 Definitions. view changes § 483.10 […]
Federal Nursing Home Quality of Care Regulations
Nursing homes that accept Medicare or Medicaid are required to comply with quality of care regulations. Although we have blogged elsewhere on specific nursing home resident rights, the current federal regulations are linked below. 42 CFR Part 483 — Requirements for States and Long Term Care Facilities § 483.5 Definitions. § 483.10 Resident rights. § […]
Long-Term Care Partnership Policies
Long-Term Care Partnership Policies One example of good planning is purchasing long-term care insurance. The greatest risk to non-taxable estates (those under $12.9 million) is the cost of long-term care. With long-term care insurance, you can shift that risk to an insurance company. A partnership policy is a special long-term care insurance policy that protects […]
CMS Announces Nursing Home Minimum Staffing Rule
[Note: Section 71111 of The One Big Beautiful Bill Act placed a moratorium on enforcement of the nursing home minimum staffing standards through September 30, 2024] On April 22, 2024, the Centers for Medicare and Medicaid Services announced a new final rule requiring minimum staffing levels in nursing homes. The new rule applies to all […]
Washington Post Reports Assisted Living Facilities Using Algorithm to Set Staffing Levels
On April 1, 2024, the Washington Post published an article titled “Algorithms guide senior home staffing. Managers say care is suffering.” The article indicates that a system, called Service Alignment, was developed more than two decades ago when assisted living facility (ALF) executives began timing caregivers performing tasks. That data was fed into a computer […]
New Report cites dangers in relying on data regarding quality of care in Assisted Living Facilities
In February 2024, Justice in Aging released a new report based on California’s “performance measure” data from the state’s Medicaid assisted living program. Aging in Justice concluded that the quality of care measures provide no meaningful information. A perfect score tells you nothing about the quality of care residents receive. The report concludes that the […]
Cost of Long-Term Care
For many years, Genworth has produced a Cost of Care Survey tracking the cost of long-term care in America. According to the survey, the projected national monthly median costs will be as follows: Homemaker Services: $5,417 Home Health Aide: $5,625 Adult Day Health Care: $1,847 Assisted Living Facility: $4,917 Nursing Home Semi-Private Room: $8,641 Nursing […]
Assisted Living Facility Not Entitled to Summary Judgment Where Cognitively Impaired Resident Filmed Nude
In Jones v. Life Care Centers of America (Tenn .Ct. Appeals 2023), a cognitively impaired resident was assisted in the shower by staff. While doing so, the employee took a call from her incarcerated boyfriend which showed the resident’s nude body. The assisted living facility moved for summary judgment after alleging the resident showed no […]

Opting Out of Arbitration Agreements
Ideally, health care providers do the right thing. Good Care is provided. There is no negligence. But what if they don’t do the right thing? What if they are negligent? Should you have the right to consider your options regarding how to hold them accountable? Over the past two decades, many long-term care providers, especially […]
Supreme Court Rules Nursing Home Resident Rights Are Enforceable Under Section 1983
Last year we reported that Talevski v. Health and Hospital Corporation of Marion County (HHC) was headed to the Supreme Court. On June 8, 2023, the U.S. Supreme Court issued its opinion, affirming the Seventh Circuit, and held that the Federal Nursing Home Reform Act (FNHRA) is enforceable under 42 U.S.C. § 1983. Justice Jackson […]
Updated Fact Sheet on Medicare Nursing Home Benefit
Medicare includes a nursing home benefit of up to 100 days following a qualifying hospital stay. The Medicare rehabilitation benefit is per spell of illness. On reason we say “up to” is because the Medicare benefit is a rehabilitation benefit and it ends when the need for skilled therapy ends. Historically, that meant Medicare coverage […]

Nursing Home Quality of Care Regulations Amended to Remove Expired COVID-19 Provisions
On June 5, 2023, the Centers for Medicare and Medicaid Services (CMS) amended 42 C.F.R. § 483.80 (infection control) and § 483.430 (Condition of participation: Facility staffing) to remove expired COVID-19 provisions. See 88 FR 36485. The specific amendments are: Section 483.80 is amended by removing paragraphs (h) and (i). Section 483.430 is amended by […]

Elder Law Mishmash June 2023
The following is a mishmash of information on various Elder Law, Special Needs Law, and Estate Planning issues. It also includes anything else we found interesting during the month of June, 2023. We will continue updating from time to time throughout the month. Last updated 6/8/2023. Keep in mind, you are using linked content at […]

CMS Oversight of Nursing Home Staffing Levels
Nursing homes are intended to be places of comfort and healing. More than 1.4 million individuals live in over 15,500 Medicare- and Medicaid-certified nursing homes across the nation. Everyone knows staffing is the most significant issue when determining whether your loved one gets the care he or she needs. Staffing levels have a direct impact […]

The Plaintiff’s Injury Case
There are many types of “Plaintiff’s cases.” This article focuses on injury cases. Injury cases can be as simple as a car wreck or as complex as a medical malpractice case. Regardless, they generally require four essential elements: duty, breach of duty, causation, and damages. See Calhoun First Nat’l Bank v. Dickens, 264 Ga. 285 […]

Should You Buy Long-Term Care Insurance
Like all insurance, long-term care insurance policies are designed to cover risk. With these policies, the risk is that you will need custodial care such as in-home care, assisted living care or nursing home care. The best thing about these policies is that they create a pool of someone else’s money you can use to […]

New Hospice Resource
On December 9, 2022, the Center for Medicare Advocacy and the National Association for Home Care & Hospice announced development of a new hospice resource. The resource is entitled “Questions to Ask When Choosing a Hospice.” You can access this resource on the CMA page or the NAHCH page.

Resident’s Right to Choose Activities and Interact with Others Inside and Outside the Nursing Home
Nursing home residents have the right to who they will spend time with and how they will spend it. Specifically, 42 C.F.R. § 483.10(f)(1) – (3), (8) provides that residents have the right to and the facility must promote and facilitate resident self-determination through support of resident choice, including but not limited to the rights […]

Resident’s Right to Refuse Unnecessary Intra-facility Transfers
Nursing home residents have a right to refuse unnecessary transfers within the facility. Specifically, 42 C.F.R. § 483.10(e)(7) and (8) provides that the resident has a right to be treated with respect and dignity, including: (7) The right to refuse to transfer to another room in the facility, if the purpose of the transfer is: […]

Resident’s Right to Share a Room; Roommates
Nursing home residents have a right to share a room with whomever they wish as long as both residents agree. Specifically, 42 C.F.R. § 483.10(e)(4) – (6) provides that the resident has a right to be treated with respect and dignity, including: (4) The right to share a room with his or her spouse when […]

Resident’s Right to Reasonable Accomodation of Needs and Preferences
Nursing home residents have a right to reasonable accomodation of needs and preferences. 42 C.F.R. § 483.10(e)(3) provides that the resident has a right to be treated with respect and dignity, including: (3) The right to reside and receive services in the facility with reasonable accommodation of resident needs and preferences except when to do so […]

Resident’s Right to Personal Possessions
42 C.F.R. § 483.10(e)(2) provides that the resident has a right to be treated with respect and dignity, including: (2) The right to retain and use personal possessions, including furnishings, and clothing, as space permits, unless to do so would infringe upon the rights or health and safety of other residents. Appendix PP: All residents’ […]

Visitation in the Nursing Home
Nursing home residents have the right to visitation. Specifically, 42 C.F.R. § 483.10(f) provides that residents have the right to and the facility must promote and facilitate resident self-determination through support of resident choice, including but not limited to the rights specified in paragraphs (f)(1) through (11) of this section. (4) The resident has a […]

Nursing Home Resident’s Autonomy
Nursing home residents have the right to make their own choices. This includes basic life choices, the right to information and to socialize, and rights concerning financial matters. Specifically, 42 C.F.R. § 483.10(f) provides that residents have the right to and the facility must promote and facilitate resident self-determination through support of resident choice, including […]

Resident’s Right to Self-Determination
Nursing home residents have the right to make their own choices. This includes basic life choices, the right to information and to socialize, and rights concerning financial matters. Specifically, 42 C.F.R. § 483.10(f) provides that residents have the right to and the facility must promote and facilitate resident self-determination through support of resident choice, including […]

Resident’s Right to Choose Attending Physician
Nursing home residents have the right to choose his or her attending physician. The physician must be licensed to practice, and if the physician chosen by the resident refuses to or does not meet requirements specified in this part, the facility may seek alternate physician participation as specified in paragraphs (d)(4) and (5) of this […]

Additional Guidance Regarding Nursing Home Patients With Cognitive Impairments
Appendix PP provides the following additional guidance regarding treatment of residents with impaired, or potentially impaired decision-making capacity: Definitions: “Court of competent jurisdiction” means any court with the authority to hear and determine a case or suit with the matter in question. “Resident representative” For purposes of this subpart, the term resident representative may mean […]

Guidance Regarding Resident’s Right to Self-Administer Medications
Appendix PP provides the following guidance regarding a resident’s right to self-administer medications as provided in 42 C.F.R. §483.10(c)(7). If a resident requests to self-administer medication(s), it is the responsibility of the interdisciplinary team (IDT) (as defined in §483.21(b), F657, Comprehensive Care Plans) to determine that it is safe before the resident exercises that right. […]

Resident’s Right to Be Informed of and Participate in Treatment
Nursing home residents have the same right to participate in the informed consent process as any other patient. 42 C.F.R. § 483.10(c) provides: The resident has the right to be informed of, and participate in, his or her treatment, including: (1) The right to be fully informed in language that he or she can understand […]

Resident’s Right to Exercise Rights
Nursing home residents have a right to exercise his or her rights as a resident of the facility and as a citizen or resident of the United States. Speficially, the facility must ensure that the resident can exercise his or her rights without interference, coercion, discrimination, or reprisal from the facility. The resident has the […]

Resident’s Right to a Dignified Existence
Nursing home residents have a right to a dignified existence, self-determination, and communication with and access to persons and services inside and outside the facility, including those specified in this section. A facility must treat each resident with respect and dignity and care for each resident in a manner and in an environment that promotes […]

Definitions Relating to Nursing Home Care
42 C.F.R. § 483.5 defines the following terms: Abuse Abuse is the willful infliction of injury, unreasonable confinement, intimidation, or punishment with resulting physical harm, pain or mental anguish. Abuse also includes the deprivation by an individual, including a caretaker, of goods or services that are necessary to attain or maintain physical, mental, and psychosocial […]

Nursing Home Resident Rights, general concepts
Nursing homes, also called skilled nursing facilities, provide a wide range of health and personal care services. Their services focus on medical care more than most assisted living facilities. These services typically include nursing care, 24-hour supervision, three meals a day, and assistance with everyday activities. Rehabilitation services, such as physical, occupational, and speech therapy, […]

Update on Talevski v. Health and Hospital Corporation of Marion County
In our August 26, 2022, News Roundup, we reported that Talevski v. Health and Hospital Corporation of Marion County (HHC) was headed to the Supreme Court. The case concerns the rights of nursing home residents. The Plaintiff argued the nursing home violated his rights under the Federal Nursing Home Reform Act (FNHRA). The nursing home […]

Elder Law and Special Needs Law News Roundup – 9-16-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]

Elder Law and Special Needs Law News Roundup – 9-9-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]

Articles – Week of September 9, 2022
We regularly scour the internet looking for information relating to elder care, special needs and elder law. Although we review a number of sources collecting information, many of the articles listed here were found using Google Scholar Alerts. If a link you need has gone missing, try pasting the link into the Wayback Machine (Internet […]

Elder Law and Special Needs Law News Roundup – 9-2-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]

Articles – Week of September 2, 2022
We regularly scour the internet looking for information relating to elder care, special needs and elder law. Although we review a number of sources collecting information, many of the articles listed here were found using Google Scholar Alerts. If a link you need has gone missing, try pasting the link into the Wayback Machine (Internet […]

Correcting the Damage Done Before You Got the Medicaid File
Taking over a case started by someone else is never my preference. It’s far easier to do something correctly the first time. So what do you do when you’re brought in to fix a case. You pray! First, if someone hires you and no decision has been made, review the file. If there is an […]

Right to Notices Regarding Medicaid from the Nursing Home
Carol and Wilbur Post are typical Elder Law clients. Carol married Wilbur more than forty years ago. Recently, Wilbur’s health declined. Wilbur has dementia and is living on Planet Alzheimer’s. Wilbur hears voices, especially when he wanders near the Post’s barn. Wilbur needs assistance with activities of daily living. Carol recently admitted Wilbur to Valley […]

Elder Law and Special Needs Law News Roundup – 8-19-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]

Articles – Week of August 19, 2022
We regularly scour the internet looking for information relating to elder care, special needs and elder law. Although we review a number of sources collecting information, many of the articles listed here were found using Google Scholar Alerts. If a link you need has gone missing, try pasting the link into the Wayback Machine (Internet […]

Elder Law and Special Needs Law News Roundup – 8-12-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]

Can a nursing home resident leave for a family meal while covered under Medicare days?
Sometimes nursing home residents want to leave the nursing home to visit family or just get some fresh are. So can they do that while Medicare is paying for skilled therapy. This question was address in a November, 2019, blog post by the Center for Medicare Advocacy. The article cites footnote of the Medicare Benefit […]

Articles – Week of August 12, 2022
We regularly scour the internet looking for information relating to elder care, special needs and elder law. Although we review a number of sources collecting information, many of the articles listed here were found using Google Scholar Alerts. If a link you need has gone missing, try pasting the link into the Wayback Machine (Internet […]

Elder Law and Special Needs Law News Roundup – 7-29-2022
We regularly post links to news articles and other resources related to Elder Law and Special Needs Law. We focus on general news, health and healthcare news, special needs news, events, government sources, financial and retirement news and legal news. Some cited resources are for professionals, but most are news or other helpful articles we […]



